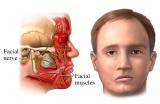
FACIAL NERVE PALSY
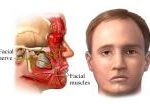
- Facial nerve palsy can be caused by numerous etiologies
- Bell’s palsy is caused by a viral syndrome in most cases
- Most patients recover all or part of the facial nerve function in months
- Maintenance of eye function is the most important consideration in the management of facial nerve palsies
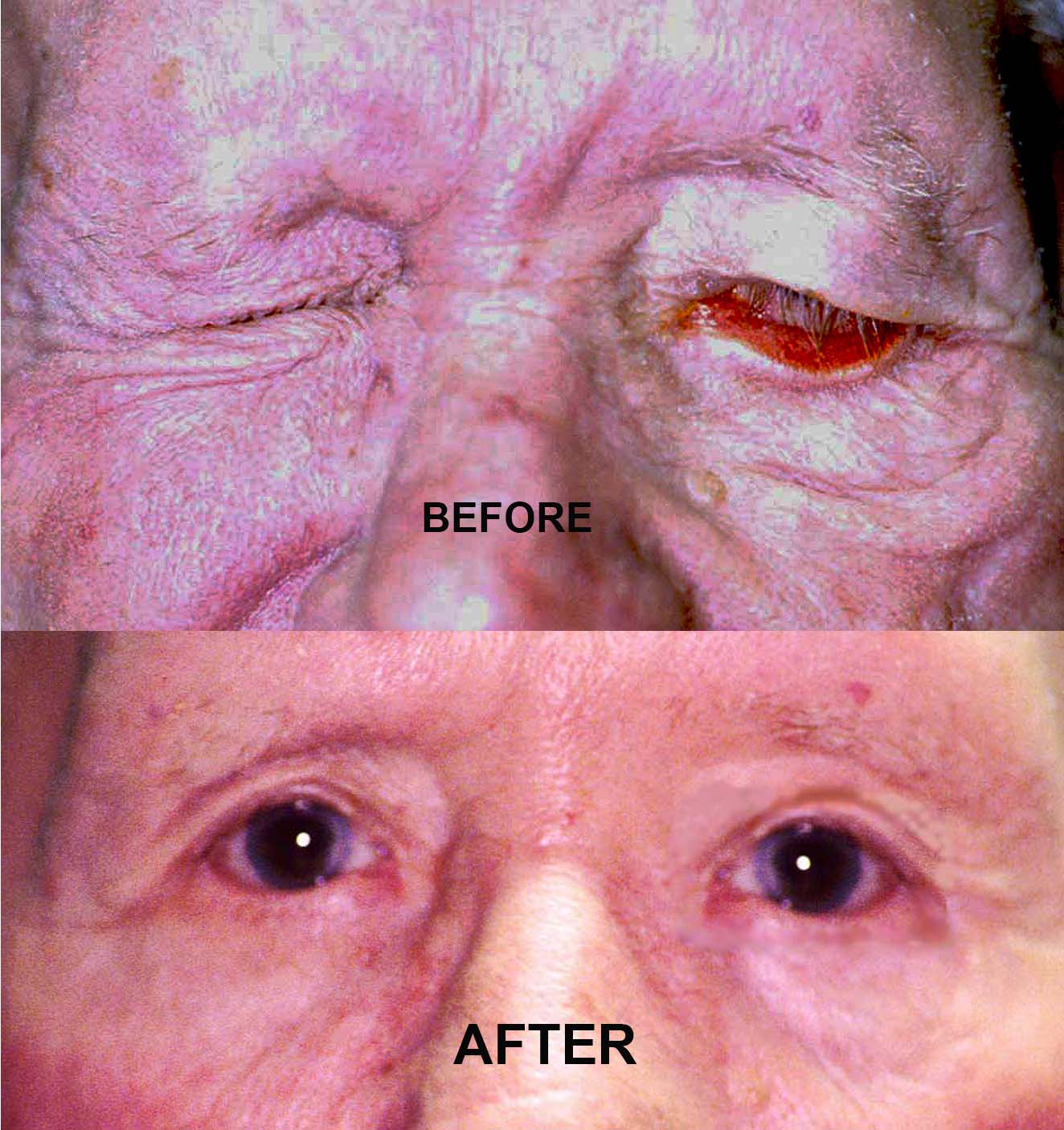
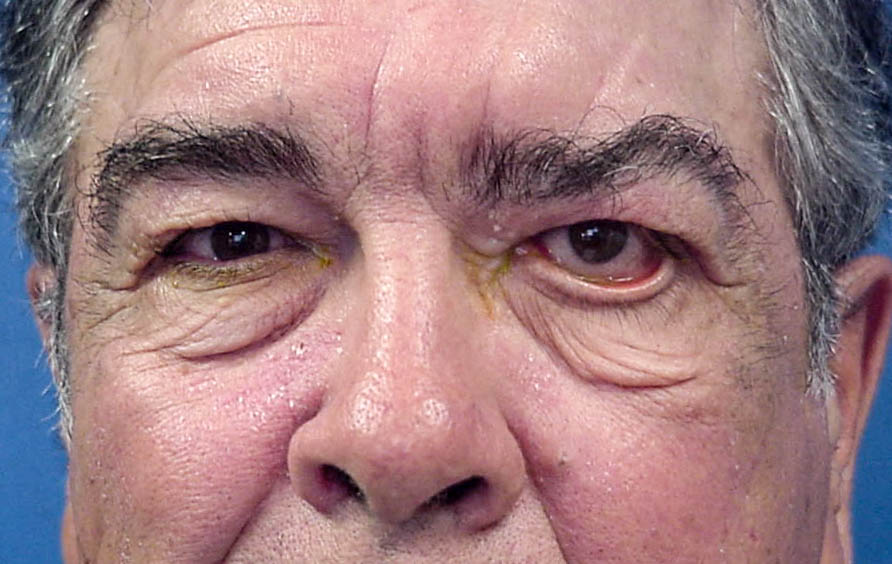
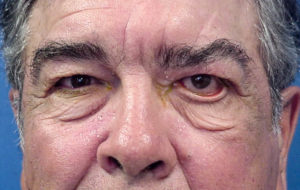
Patients with a facial nerve palsy can be greatly disabled by the signs and symptoms associated with such a paralysis. Manifestations include: drooling, loss of facial tone and symmetry, eyebrow and forehead ptosis, secondary dermatochalasis, lower eyelid ectropion, loss of the lacrimal pump with epiphora, decreased blink reflex, decreased tear production, dry eye, upper eyelid retraction, corneal exposure, corneal ulcer, decreased vision, loss of the corneal squeegee effect, and facial atrophy.
Frequently, facial nerve palsies are transient in nature with minimal long term sequelae. Occasionally, the palsy may be long term with prolonged and disastrous consequences. Obviously, the etiology, prognosis, and the manifestations of the palsy determine which management options will be employed. Conditions which affect lacrimation or corneal sensation are more likely to threaten sight than facial nerve lesions that cause only a simple motor palsy.
Preoperative Evaluation
Patients with a facial nerve palsy must undergo repeated and complete eye examination. Particular attention is paid to the specific cause of the facial nerve palsy, the duration and associated symptoms. The examination will focus on the tone and position of the eyelids. Specifically, the amount of closure of the lids is noted as is the rapidity and completeness of the blink. The laxity and tone of the lids is also noted. The position of the tear drainage apparatus and the presence of eyelid deformities are noted. A biomicroscopic examination is performed detailing the state of the surface of the eye including: the tear film, the oil glands in the eyelids, the conjunctiva and the cornea. Quantitative measurement of the tear film layer is performed.
In many cases patients can be managed medically with topical lubricants. This includes one of the variety of topical over-the-counter lubricants. While there are some important subtle differences in these different medications, the major distinction is in the “thickness” of the lubrication. Most patients require lubrication with an ointment at bedtime and possible taping of the lids shut at night. Some patients require moisture chambers as well. It is not infrequent that we place punctal plugs to block the tear drainage system and therefore provide more “wetness” to the cornea. For patients that fail these medical treatments we offer surgery.
The Surgery
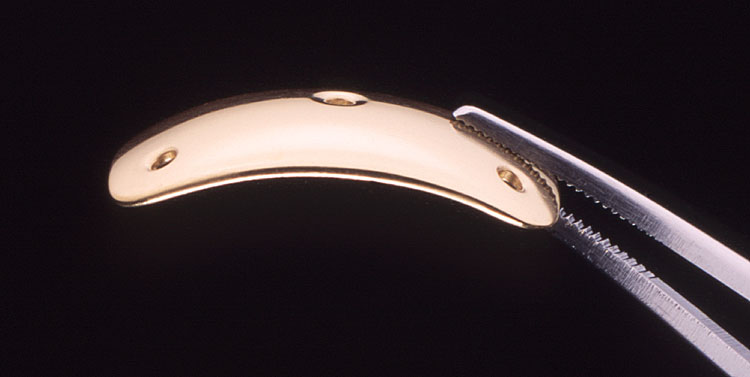
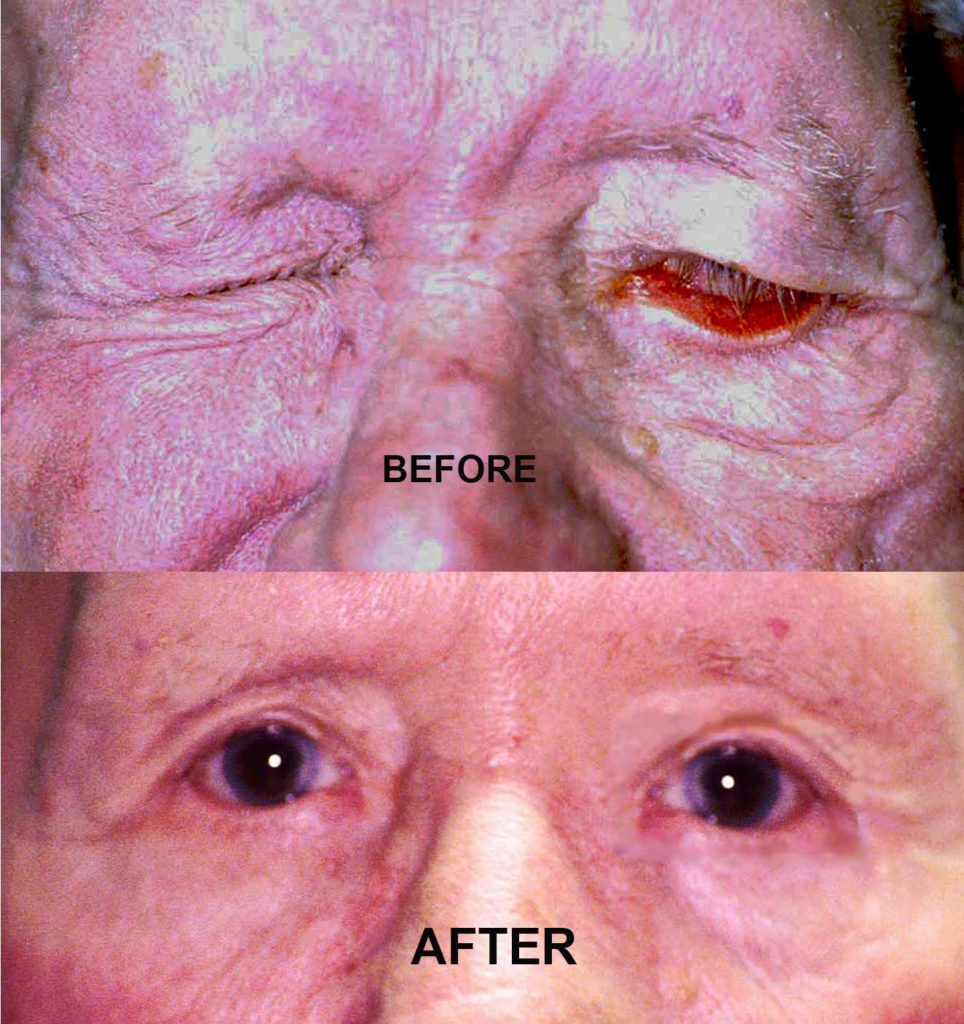
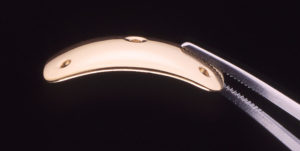
Over the last several hundred years a wide variety of techniques have been used to rehabilitate patients with facial nerve palsy. Each of these techniques is associated with unique complications. One of the simplest methods of treatment is placement of an externally taped lead weight to the upper eyelid. Should this provide relief to the patient we often times will offer placement of a gold weight inside the upper eyelid. This procedure is done under local anesthesia and takes approximately 30 minutes. The gold weight is removable should the patients symptoms subside.
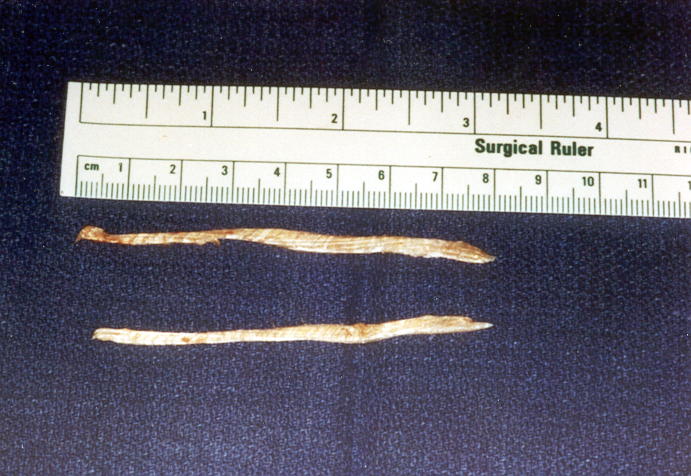
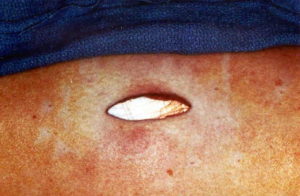
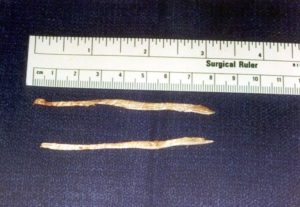
Frequently, patients with facial nerve palsies require “tightening” of the lower eyelid. This can be done simply as an outpatient procedure. Occasionally, patients with severe and long standing facial nerve palsies require a more definitive operation. For these patients we perform an encircling procedure of the upper and lower eyelids with either silicone bands or “fascial” tissue bands. This provides adequate eyelid support, adequate corneal protection and for reanimation of the eyelids. These procedures are also done on an outpatient basis and take approximately 1-2 hours.
Postoperative Care
With any of the above procedures patients can expect swelling and bruising. The patient may be instructed to clean the wounds 1-2 times daily with sterile saline or hydrogen peroxide solution. Antibiotic ointment is placed on the wounds and in the eye several times daily. Many patients are placed on oral antibiotics in the immediate postoperative period. The first postoperative evaluation will be on day 5-7. Most postoperative swelling resolves in the first two weeks.
Complications
Complications are rare with facial nerve palsy surgery for the eyelids. Complications include but are not limited to the following: bleeding, infection, scarring, eyelid deformity, need for additional surgery and rarely loss of vision. Most experts believe the risk of loss of vision to be 1/40,000. Should you experience significant bleeding, pain or change in your vision, you must contact your physician immediately.
CONTACT
PAY MY BILL - DR. GILLILAND
FInd US
© 2020 GRANT GILLILAND MD. All Rights Reserved.